By John Christodouleas, MD, University of Pennsylvania; Mary Feng, MD, University of California San Francisco; Charles S. Mayo, PhD, University of Michigan; and Kristy Brock, PhD, MD Anderson Cancer Center
In 2018, ASTRO published Minimum Data Elements for Radiation Oncology: An ASTRO Consensus Paper (MDE) in response to requests for required radiation therapy (RT) data. During the development process, ASTRO learned that a parallel exercise was occurring at ASCO, which resulted in the mCODE (minimum Common Oncology Data Elements) standard. In June 2019, ASTRO joined the Executive Council of mCODE and, later that year,CodeX (Common Oncology Data Elements eXtension), an initiative focused on creating new oncology data standards.
Prior to ASTRO’s involvement in these initiatives, limited standards existed, aside from DICOM, that could transfer data outside of radiation oncology (RO) systems. ASTRO utilized MDE to create a CodeX use case focused on standardizing the data elements required for an end of treatment (EOT) summary. ASTRO’s role has been that of a convener and, currently, the RO CodeX use case includes four specialty societies, three academic institutions, three electronic health record (EHR) vendors, three data transfer groups and representatives from the National Cancer Institute (NCI).
To date, the CodeX project has created more than 300 new RO-specific data elements. These concepts have been added into the mCODE standard, which is being adopted by health care institutions and vendors nationwide and have been approved for new SNOMED codes. These standards and relationships have been developed in conjunction with vendors who are currently working to develop a framework for data transfer that aligns to federal interoperability mandates.
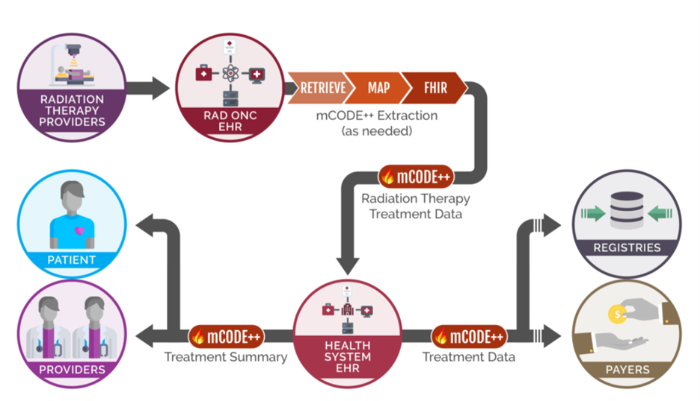
CodeX Radiation Therapy Treatment Data for Cancer conceptual map.
Improved data collection for a variety of quality and research programs
While the EOT focus is useful to alleviate a common pain point in practices, the work can easily translate to other domains, including data collection for the upcoming RO Model, clinical trial data and improving the data collection for a variety of cancer programs.
National cancer registry programs in the U.S., like the NCI’s Surveillance, Epidemiology, and End Results (SEER) Program and the Commission on Cancer’s National Cancer Database (NCDB), collect data by leveraging the infrastructure of the national cancer surveillance system, which mandates the reporting of information on cancer diagnoses and treatments to state and federal surveillance programs. Such registries form the basis for programs that track patterns of care and create clinical research repositories. These have been very fruitful for the community, producing over 2,000 RO papers in the last five years using data from SEER or the NCDB despite both registries containing only limited RT data. The NCDB, which has more RT data elements than SEER, historically only collected that a treatment occurred: a single field for body site and a single field for radiation dose. There is interest in capturing more treatment details, but this currently requires manual abstraction of data from the EOT summary. Registries will benefit from the CodeX effort because it will drive standardization in the format and vocabulary of the EOT summary that is captured in the patient’s medical record.
Standards are also vital to research. The importance of precision medicine using advanced computing, machine learning and artificial intelligence (AI) was highlighted at an NCI and Department of Energy virtual workshop in March 2021. The engagement of the attendees, and extensive lists of identified priorities, clearly indicate that big data, the development of standard nomenclature and the ability to share data between cancer centers is critical to the further development of AI to advance the precision of RO. The mCODE standard is already being utilized in oncology clinical trials. Data standards will improve the collection of high-quality data in the EHR that is complete, accurate and computable, to support transformative goals employing statistical and machine learning methods to point the way to better clinical insights.
The initial CodeX goal is to connect vendor information systems; however, the proposed interface will also eventually serve as a connection between RO information systems and other cancer data repositories. Such a connection will create a pipeline of more accurate and comprehensive data summarizing a patient’s radiation treatment, increasing the power and value of these repositories.
The importance of leveraging partnerships
Constructing large, comprehensive data sets from “real world” data holds the promise to enable learning from each patient and how to better care for future patients. A substantial barrier to creating multi-institutional databases is the lack of RO standards, which impedes our ability to coalesce technical efforts in constructing interoperable systems to aggregate this data.
The development and success of the CodeX use case has been due, in part, to the tremendous collaboration between ASTRO and the American Association of Physicists in Medicine (AAPM), who joined CodeX in 2020. Many of the new standards, specifically in modality, technique and treatment site, were based on this joint effort. This began with the 2017 Red Journal publication of the Task Group 263 (TG-263) report on standardized nomenclatures, developed to support treatment planning. TG-263, led by AAPM, combined the multi-disciplinary efforts of members of multiple professional societies into the development of consensus-based standardizations. This marked a shift from standards being imposed by others outside of RO toward standards that fit into routine practice because they were developed with the expertise of our members.
Following in the footsteps of these efforts, the operational ontology for radiation oncology (OORO) is being constructed to address additional gaps in data standards. While operating under AAPM, it is carried out in partnership with ASTRO and utilizes the insights and skills of physicians, physicists and other professionals. This collaboration of professional societies has paid dividends, with consensus-based development of value sets and standards that support the needs of radiation oncology. The OORO will be the inevitable pipeline for further standards development using the CodeX infrastructure.
Radiation oncology relies on complex hardware and software systems to provide and coordinate the best possible care for patients. At the system boundaries, information is exchanged and if these are not clearly defined, the safety and efficiency of clinical care may be compromised. Integrating the Healthcare Enterprise – Radiation Oncology (IHE-RO), from AAPM in collaboration with ASTRO and other organizations, comprises physicists, physicians, software engineers and others from clinical practice and industry working to identify and solve connectivity issues to ensure safe, efficient radiation treatments by improving system-to-system connections.
Utilizing its strong collaboration with industry partners, IHE-RO is acting on the standards created in CodeX to build the infrastructure necessary to exchange these data between the RO systems and broader EHRs to bolster care coordination. End-to-end testing will be conducted during Connect-a-Thons to test the success of product development and their integration. This is crucial to ensure that the development of standards becomes a reality for end users.
The growing, and successful, body of work emerging from our professional societies acting in concert clearly demonstrates the success of working together, serving the interests of all members.
Future vision
While RO standards development is focused on the EOT summary now, there is the potential to create many secondary gains for the global RO community. One can envision how CodeX and the mCODE initiative could enable international comparisons of patterns of care, clinical guideline adherence or the creation of large and international research repositories. In this way, the work ASTRO and AAPM are doing now could create benefits far beyond the primary mission.
For any questions regarding these initiatives, please email ASTRO’s Senior Quality Improvement Manager Randi Kudner.


